Advanced Dementia – The Silent Killer
How Project Dignity is Giving Voice to Our Silent Sufferers
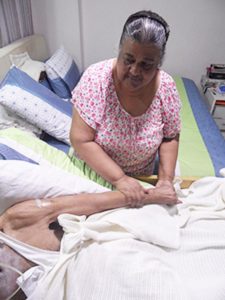
Auntie Rose giving an arm massage to Uncle Din, as part of her care-giving routine.
Ian Yip, Dover Park Hospice (with inputs from Adj Assoc Prof Allyn Hum – Married for almost 28 years, Auntie Rose, 71-years-old, and Uncle Din, 83-years-old, led fairly active lives. Uncle Din would jog around the estate or go for walks, and he would pull along Auntie Rose to accompany him so that she would get her exercise as well.
However, life became very different for the once-active Uncle Din, especially after a series of falls. One such fall, which occurred almost seven years ago, fractured his hip bone and he had to undergo surgery. Then in 2012, Uncle Din was diagnosed with Alzheimer’s and Dementia. And in the short span of a few years, his condition deteriorated very quickly. Now, Uncle Din lies immobile in his bed with a feeding tube attached.
“Din always did all the marketing and paid the bills,” Auntie Rose reminisced. “He loves to walk and to cook. We always go for our walks and to sight-see. I can’t believe he is like this now,” Auntie Rose bemoaned. “I feel very sad to see him in this condition. Sometimes he cries … You can see his tears rolling down his cheeks. He can still hear and see but he can’t talk.”
Uncle Din’s condition is characteristic of patients diagnosed with Advanced Dementia (AD).
Dementia is a neurodegenerative condition that causes a long term and gradual decrease in a person’s ability to think and remember. “It affects memory and the ability to care for oneself. As the disease progresses, one becomes physically immobile to the point of being bed-bound,”
Dr. Allyn Hum, a visiting consultant at Dover Park Hospice (DPH) and Senior Consultant at the Department of Palliative Care at Tan Tock Seng Hospital (TTSH), explained. “Many of our patients lose independence and autonomy to speak for themselves. Consequently, the burden on the caregivers will increase due to such losses.”
Dr. Hum highlights the programme’s mission at DPH: to reduce the symptoms and burden of these patients who are unable to speak for themselves, to give a voice to their suffering that is often not recognized and addressed.
“We physically examine the patient, look out for signs and symptoms of their suffering,” she elaborated. “We also teach families and caregivers how to look after their loved ones, and how to anticipate and manage complications related to Advanced Dementia (AD), for instance, infections; pressure sores; feeding issues; and how to care for themselves. We use specific assessment tools that empower both professional and familial caregivers to be more attuned to our patients’ needs,” she said.
“This is particularly important for advanced dementia patients as their burden of suffering may be just as great as advanced cancer patients, but this is just not recognized,” Dr. Hum continued. “At the same time, many healthcare professionals are not cognizant of the fact that advanced dementia is also a terminal illness.”
This issue is further compounded by the current model of palliative homecare which is based on cancer, and “may not fully address the needs of the AD patients who are typically not very responsive at the end stage of their illness, and thus, cannot speak or advocate for their own needs. We need to advocate for these “silent sufferers and continue to dignify their lives.”
Complications at this stage of their lives are often addressed by admission to the emergency room and hospital, Dr. Hum elaborated. “However, these interventions neither relieve suffering nor improve quality of life. Hence, the intent is to offer the option of support within their homes, with care in a familiar and comfortable environment. In so doing, there will be judicious use of healthcare resources, with potential reduction in the number of Emergency Department visits; decrease hospital admissions and re-admission rates. This helps to reduce cost, time and emotional burden placed on caregivers.”
For many patients with AD, the agonizing problem is that they cannot articulate their needs, which translates into physical suffering which is not identified. “Many of our patients may express discomfort by being restless or being verbally aggressive, and this can be misconstrued as being difficult,” Dr. Hum added.
Many caregivers also find it extremely challenging to care for their loved ones at home as the AD patients have complications such as eating issues, infections, and myriad of other symptoms. More often than not, caregivers feel very burdened as they are not certain if they are making the right decisions for their loved ones at home or not. Project Dignity hopes to change that over time.
“These are issues we are able to address, and if the outcome is that patient’s comfort is maintained, caregivers supported, plans of care proactively established, care can be continued at home,” Dr. Hum said. ”In addition, plans of care are made with the numerous families so that patients can continually be cared for at home, in the hospital, or at the hospice, which are essential components of family support. The team also regularly makes phone calls to check on the patient and families in between its home visits. The eventual aim is to spread this service nationwide so that more advanced dementia patients and caregivers can benefit.”
Although this pilot project seems small in scale, the work that the Project Dignity Team has been performing, together with the DPH Home Care Team, is critical and beneficial to primary caregivers who attend to their terminally-ill loved ones at home, and who suffer in silence.
Since its launch in October 2014, Project Dignity; a special patient-centric initiative, which DPH had embarked on since October 2014, has provided Palliative Care to more than 120 home-bound, advanced dementia patients.
The Project Dignity Team includes Dr. Erwin Francisco, Resident Physician; Ms. Felicia Lam, Nurse Clinician; Ms. Koh Tang En, Medical Social Worker; Ms. Tay Ri Yin, Research Assistant; Ms. Yoong Jia Horng, Programme Manager; and Dr Allyn Hum. This programme is a partnership between Temasek Cares, DPH, TTSH, and the Agency for Integrated Care (AIC). It is open to all Singaporeans and PRs who have been referred by their doctor in TTSH.
It is the hope that this programme will continue to expand as Singapore’s greying population continues to grow, as well as to continue assisting, supporting even more caregivers and helping them meet their loved ones’ needs as they spend their remaining days in the comfort of their own homes.
DEBUNKING THE MYTHS SURROUNDING DEMENTIA
Myth: Dementia is a natural part of ageing.
Truth: Dementia does not necessarily occur when a person ages – it is a medical condition. If it were a natural part of aging, then everyone over the age of 65 would have it. However, it is estimated that dementia affects 5% of the population older than 65, with the rates rising with increased age. Millions of people age into their 80s and 90s without much memory decline.
Myth: Once you have dementia there is nothing you can do.
Truth: Dementia is a progressive disease, meaning it continues to get worse the longer one has it. However, there are steps people can take to slow the progression of dementia and to make life easier for those suffering from it.
Myth: Only the elderly get dementia.
Truth: While dementia is indeed much more common in the elderly, there are also cases where it occurs in younger people, as young as in their 30s. Dementia can occur as a result of brain damage due to a head injury, stroke, alcohol abuse, or brain infection to name a few; causes that aren’t necessarily related to ageing. About 5-10% of people with Alzheimer’s disease have early-onset Alzheimer’s, which typically develops in a person in his/her 50s.
Myth: People with dementia can’t understand what’s going on.
Truth: Many people believe that a person with dementia cannot communicate what they can’t understand or what’s going on around them. This is not true. The part of the brain that is responsible for communication is different from the part of the brain that deals with awareness. So, while they might have difficulty communicating, they still most likely do have ideas to communicate and can understand the situations they are in.
Myth: There is nothing I can do to lower my risk of dementia.
Truth: There are many things that have been shown to help decrease your risk of developing dementia, such as exercising often, eating healthy (lots of vegetables and fruit, cutting back on fats), and making use of mental abilities through puzzles, reading, and learning new skills.
Myth: There is a cure for dementia.
Truth: While there are methods for helping people cope with dementia, there are currently no cures for it. The best that can be done is improving one’s quality of life and management of symptoms.
Myth: Someone with memory loss must have dementia.
Truth: Once someone reaches middle age, most will experience a slight decline in their memory and this is considered a natural part of ageing. In order to be diagnosed with dementia, one must manifest multiple symptoms, not just memory loss alone.
Myth: My loved one remembers certain things, so they must not have dementia.
Truth: Different forms of dementia can affect different aspects of a person’s memory. So, just because they can remember certain things does not mean that they don’t have dementia.
Myth: People with dementia are oblivious to their symptoms.
Truth: In the early stages of dementia, it is common for people to realize that their memory is becoming worse and that they may be having trouble completing certain tasks. It varies from case to case, and even with each person, it can vary from hour to hour. Depending on the person, it may be okay to help them be more aware of their symptoms, but as the dementia progresses, it is probably best to not point them out. Awareness of the symptoms declines as dementia progresses to further stages.
Myth: Dementia results in aggression or violence.
Truth: While it can occur, each person’s experiences with dementia are different, and aggression is less common than you might think. Patience, good communications, and keeping notes about the behaviours of a person with dementia can all help reduce the risk of aggression. While a person with dementia can have difficulties communicating, they still can send signals at their current state. Aggression would only show when there is something that is making them uncomfortable. As such, by exploring the circumstances of their aggression, a caregiver can usually determine what’s wrong.
Source: Advanced Dementia – The Silent Killer. Dover Park Hospice




